It was the last Friday of the school holidays, and for eight-year-old Bridgette, it should have meant a McDonald's dinner and a sleepover with her school friend Neve.
Instead it would be the start of a long, painful bout of leukaemia.
After pulling into the driveway with the takeaway meal, Bridgette's mother would watch her daughter and Neve wander inside with their takeaway before being met by her husband, Steve, who grabbed her and broke the news he'd just received.
Bridgette has leukaemia, we need to take her to the hospital right now. She needs a blood tranfusion. Monash Emergency is waiting for her.
"I just couldn't believe it. My whole world was shattered in that instant. I couldn't understand what he was saying to me," Sharon Veneris, Bridgette's mother, told The Huffington Post Australia.
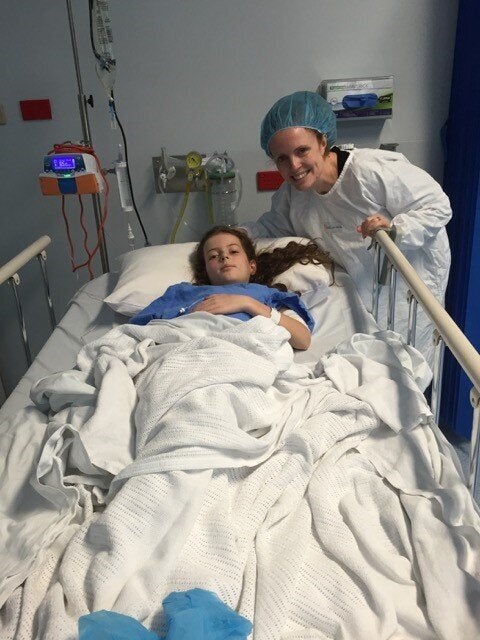
What followed was an eight-day stint in hospital, a port in her chest and the start of chemotherapy treatment.
But it could have ended much worse.
According The Leukaemia Foundation, in acute or aggressive cases, the patient can require immediate and intensive treatment, often within 24 hours of diagnosis.
"Bridgette would have been dead if we'd have waited the weekend to get her blood test results," Veneris said.
Weeks prior, Bridgette, a grade-three student who loved school, tennis, swimming and dance had been complaining of tiredness and lethargy. After a trip to the GP they were told she was probably low in iron. No blood test was ordered.
With no improvements and a family holiday booked to Bali during the first week of school holidays, Veneris decided to book Bridgette into a clinic for further testing upon their return.
"The results showed that she needed a blood transfusion and to be treated right away. Her condition was fatal," Veneris said.
The results showed that she needed a blood transfusion and to be treated right away. Her condition was fatal.
It was Dr Ellen Maxwell, a Melbourne haematologist who analysed Bridgette's blood that Friday night.
With the doctor who had ordered Bridgette's tests away for the weekend, Maxwell would be the one to personally call Bridgette's father, Steve, and instruct him of the leukaemia diagnosis and that his daughter would need an emergency blood transfusion.
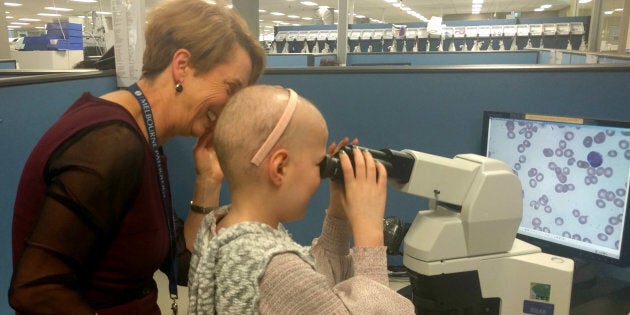
Fast-forward one year and Bridgette, now 12 months into her chemo treatment, has met with Dr Maxwell for the first time.
It was no chance meeting, but something Bridgette had been looking forward to, in some ways even before her diagnosis.

"Bridgette was actually interested in haematology before she got sick," Veneris said.
In fact, the December before her diagnosis she had asked for a microscope from her grandparents for Christmas.
"She used to put all sorts of strange things underneath -- a leaf, bugs and then one day she asked her dad to prick his finger so that she could look at his blood," Veneris said.
Both Sharon and Steve had tried to reach out to Maxwell a few days after Bridgette's life-saving blood transfusion.
"We rang Melbourne Pathology and asked to speak to the person that saved our daughter's life, we wanted to thank her," Sharon said.

But the pathology unit couldn't give out details for privacy reasons and said they would pass it on and also keep it on file.
Months later, Sharon and Steve would hear from Melbourne Pathology who had agreed to facilitate a meeting between Bridgette and Maxwell, after hearing of Bridgette's passion for haematology.
Bridgette has pictures on her wall of what healthy blood should look like and what leukaemia looks like from research we've done on the Internet, but today she got to see what it looks like in real life.
On Wednesday Maxwell shared with Bridgette the slide of blood that showed her original leukaemia cells.
"Bridgette has pictures on her wall of what healthy blood should look like and what leukaemia looks like from research we've done on the Internet, but today she got to see what it looks like in real life," Veneris said.
Despite Bridgette taking another turn after receiving new treatment, it didn't take away from her excitement to meet Maxwell and ask her questions about how she can get into her line of work.
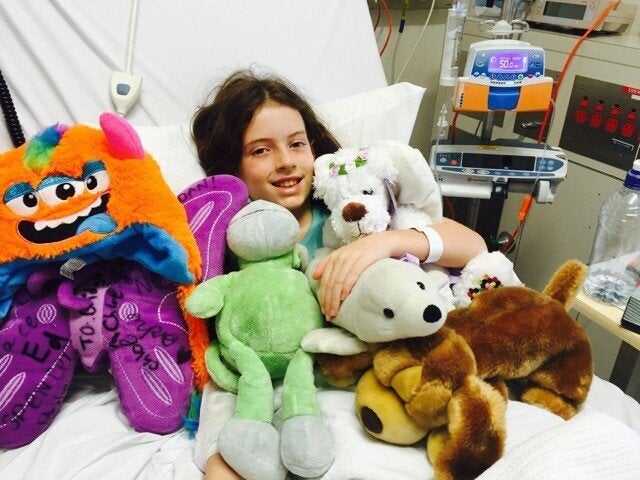
"She's been very sick with ulcers all down her throat and had to have another blood transfusion last week. But all she's just kept saying is, 'I hope I'm well enough in time to be ready for this opportunity'," Veneris said.
Bridgette tries to go to school when she can, but often when she is absent she's too sick to do any work at home which has meant she's missed out on a lot of things.
"She can no longer play tennis or do any of her extra curricular activities," Veneris said.
You miss out on so many things but at the same time we're just grateful that she's still alive and here with us.
She can't do dancing or calisthenics, violin or singing. And no swimming lessons either, as she is not allowed to go in the pool for fear of infection.
"You miss out on so many things but at the same time we're just grateful that she's still alive and here with us," Veneris said.
More than 13,000 Australians are expected to be newly diagnosed with blood-related disorders this year -- equivalent to 35 people each day.
For Sharon and Steve, getting the chance to thank Maxwell for her quick actions in person, was something they've been hoping to do for some time.
"The general public should know what amazing work the pathology units and people in the lab coats actually do."
"It's not just doctors, nurses and oncologists, but there are people working behind the scenes, 24 hours a day who analyse blood and are really saving lives."
"Just because we don't see them, doesn't mean they deserve any less credit," Sharon said.