One in four adults have had the cervical cancer-causing human papillomavirus at one point in their lives, but a new breakthrough led by the creator of the Gardasil vaccine could stop the virus before it causes cancer.
Professor Ian Frazer won the Australian of the Year award for the creation of the Gardasil vaccine, which gives immunity from about 75 percent of human papillomavirus (HPV) strains and now he's working on another vaccine to treat those who are already infected.
HPV is one of the most common viruses on the planet -- most people don't even know they have it and it is often sexually transmitted. In some women, however, it can have concerning consequences as the virus causes abnormal cells in the cervix -- which often show up in an abnormal pap smear -- and can lead to cervical cancer if left untreated.
The vaccine's take-up is about 70-75 percent in Australia among young people but even in the U.S. where uptake is lower, Frazer told The Huffington Post Australia rates of the virus had declined.
"Abnormal pap smears for women under 30 are almost gone," Frazer said.
"It's not a highly infectious disease so if you can get half of the population vaccinated, there'll be a significant decline."
But Frazer didn't stop.
Gardasil was unable to help people already infected by HPV.
Dr Ian Frazer.
He's working with healthcare research group Admedus Ltd in the creation of a DNA vaccine which could be injected in people who already have the virus, and flag it in a way so that the body destroys it.
Animal model trials on mice were promising and the next step was human trials. If it works, will cervical cancer be a thing of the past?
"Well that's the hope, yes," Frazer said.
"We've had very promising results and we don't know how the next trial will go but the results do look very good."
Frazer said there was a chance the DNA vaccine could also be used in conjunction with other treatments for people who already had cervical cancer "but that's more complicated".
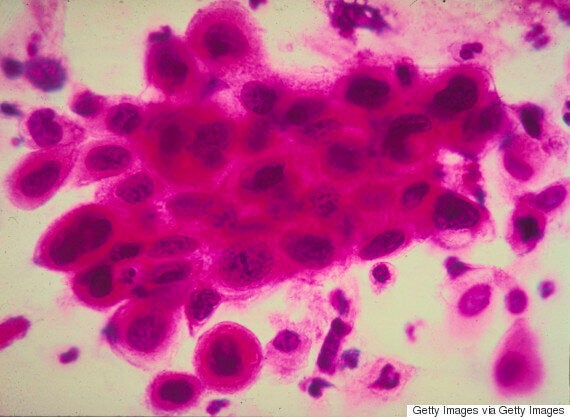
A close-up of cancer cells in the cervix.
In terms of how the DNA vaccine would work, Frazer said it came down the the fact that HPV wasn't passed from the body like any other virus.
"It’s quite simple really, most viruses kill the cells they infect, which is a nasty danger signal for the body so it turns on its defences pretty quickly to kill it and then kill the cells making more of the virus. This process saves us from flu and a whole range of different infections.
"Human papillomavirus doesn't kill the cells it infects -- rather it make them grow more. There's no danger signal to body -- all the body sees is tissue repairing itself."
The DNA vaccine takes a viral protein and alerts the body to the fact that it's dangerous. Once the vaccination is injected, the body now sees this particular protein as dangerous, and sets to work destroying the cells with this protein -- which is where the virus is.
Admedus is also looking at developing a similar vaccine for the herpes simplex virus 2 which causes genital herpes.
Chief Scientific Officer Dr David Rhodes said the technology developed by Admedus in conjunction with Frazer could potentially be applied to a range of viruses, bacterial infections and cancers in the future.
A previous version of this story incorrectly named Admedus LTD as Admedus Australia Medical Technologies.