In the UK, one in five children and one in 12 adults have eczema, but despite the common nature of the skin condition, it can leave sufferers feeling self-conscious.
Blogging about his experience of living with eczema on HuffPost UK, youth activist Liam Beattie said: “Eczema may on appearance appear to be nothing more than physical damage, [but] it has a real effect on people’s mental health and overall wellbeing.
“Growing up I fought endless battles to overcome the insecurities I had over my appearance. It wasn’t just that I didn’t want others to see me, I would go as far to avoid looking at myself in mirrors in shops.”
Charities around the UK are raising awareness of the condition so that sufferers like Beattie feel less ostracised and others better understand the condition.
So whether you have eczema and want to learn more, or you’ve spotted a friend or colleague with sore skin, here’s what you need to know.
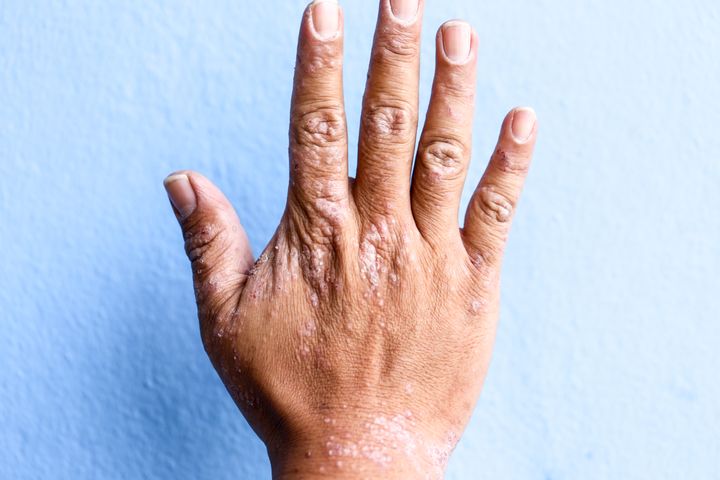
What is eczema?
Eczema is a non-contagious dry skin condition where symptoms and severity differ from person to person.
While there are several different types of eczema, atopic eczema (also known as atopic dermatitis) is by far the most common.
“Atopic eczema is an inflammatory condition of the skin characterised by dryness and itching. It can affect both men and women equally and usually presents in the first weeks or months of life,” Dr Anjali Mahto, consultant dermatologist and British Skin Foundation spokesperson told HuffPost UK.
“In simple terms, the skin barrier in patients with atopic eczema doesn’t work very well, which means irritants can enter the skin causing inflammation and dryness of the skin.”
According to the NHS, other types of less common eczema include:
discoid eczema – eczema that occurs in circular or oval patches.
contact dermatitis – eczema that occurs when the body comes into contact with a particular substance.
varicose eczema – a type of eczema that affects the lower legs and is caused by problems with the flow of blood through the leg veins.
seborrhoeic eczema – eczema where red patches develop on the sides of the nose, eyebrows, ears and scalp.
dyshidrotic eczema (pompholyx) – eczema that causes tiny blisters to erupt across the palms of the hands.
What causes atopic eczema?
Dr Mahto explained that the cause of eczema is still not fully understood, but it tends to run in families and often develops alongside other conditions, such as asthma and hay fever.
“Eczema cannot be ‘caught’ from other people. Everyday life is filled with triggers that can make eczema, or the associated itching, worse, so care should be taken to minimise or avoid exposure to them,” she said.
“Some of the main culprits include heat, dust, soap and detergent. Being
unwell (such as having a cold), infections, stress and dryness of the skin can all cause flare ups.”
The NHS advises that women may find their symptoms get worse in the days before their period or during pregnancy while others report that their symptoms get worse when the air is dry, such as in the winter months when we’re exposed to central heating.
According to Dr Mahto, in a small percentage of cases eczema can also be linked to diet and it is therefore worth keeping an eye out for any patterns in your diet that seem to be linked with flare ups.
“Potential culprits include dairy products, chocolate, eggs, peanuts, citrus fruits and colourings,” she said.
What foods can help atopic eczema?
Dietician Dr Sarah Schenker, who works with the eczema cream brand Cetraben, said that including adequate intakes of vitamin D within your diet can help ease eczema symptoms.
“This can be found in oily fish which provides vitamin D and also ensures a good intake of omega 3 fats. Probiotics and prebiotics may also help manage eczema, they can be taken either as a food supplement or from increasing food sources in the diet, such as live yogurts, wholegrains and green leafy veg,” she said.
Dr Schenker added that eating foods in vitamin C is essential for healthy skin, particularly if you’re prone to conditions such as eczema.
“One of its [vitamin C’s] most important roles in the body is in the production of collagen, a protein needed for wound healing,” she explained.
“It is also an important nutrient for the immune system which fights off invading bacteria and viruses and protects against disease. Healthy skin is dependent on good immunity.”
Some forums also suggest cutting back on alcohol can be central to improving eczema symptoms as drinking alcohol dehydrates the body and therefore dries out the skin, potentially increasing uncomfortable cracks and itching.
What treatments are available for atopic eczema?
Your GP may be able to help you to identify triggers that make your eczema worse, meaning these can then be avoided as much as possible.
However, Dr Mahto said you may still need to use an emollient, which can come as a lotion, cream or ointment, in order to ease symptoms of dryness and itching.
“Speak with your doctor or dermatologist who will help find the best emollient
for you and your skin. It’s often a case of trial and error to see which works best for each patient,” she said.
“In more severe cases topical steroids, antibiotics and antiseptics, topical
immunosuppressants or UV light treatment can be used to treat eczema.”
Dr Mahto added that while emollients will help to keep skin moisturised, you should also be sure to use fragrance-free soaps, which can often make symptoms worse.
“Don’t wash more frequently than necessary and wear non-irritating fabrics such as cotton,” she said.
“Most importantly try not to scratch as broken skin can let bacteria in, which can cause infection.”
If living with eczema is affecting your mental health, speak to your GP who may refer you for CBT (cognitive behavioural therapy), or speak to one of the mental health charities below.
Useful websites and helplines:
- Mind, open Monday to Friday, 9am-6pm on 0300 123 3393
- Samaritans offers a listening service which is open 24 hours a day, on 116 123 (UK and ROI - this number is FREE to call and will not appear on your phone bill.)
- Get Connected is a free advice service for people under 25. Call 0808 808 4994 or email: help@getconnected.org.uk